Traditional Chinese Medicine does not have a single category called "perimenopause." It has something more precise: a system of pattern identification that can distinguish between dozens of different presentations of the same underlying transition, each requiring a different treatment protocol.
This is TCM's primary advantage. The same symptom — a hot flash, for example — can arise from Kidney Yin Deficiency, Liver Qi Stagnation, Heart Fire, or Phlegm-Heat obstructing the channels. The treatment for each is different. Getting it wrong wastes time. Getting it right can produce changes within weeks.
## The TCM Framework for Perimenopause
In TCM, the transition Western medicine calls perimenopause corresponds to the completion of the 7th life cycle — the 49th year, when Tiangui, the "heavenly water" governing reproductive function, begins its inward return. This is not a deficiency to be corrected. It is a completion to be supported.
The primary organs involved are the Kidney (which governs essence, reproduction, and the life cycle), the Liver (which governs the smooth flow of Qi and is particularly vulnerable in women), and the Heart (which houses the Shen, or spirit — explaining the emotional and cognitive symptoms of perimenopause).
Common TCM patterns in perimenopause include:
**Kidney Yin Deficiency** — the most common pattern. Hot flashes, night sweats, dry mouth, insomnia with restless dreams, lower back ache, urinary frequency.
**Kidney Yang Deficiency** — chilliness, fatigue, depression, low libido, urinary incontinence, weight gain.
**Liver Qi Stagnation** — irritability, emotional volatility, breast tenderness, irregular cycles, sighing.
**Heart-Kidney Disharmony** — anxiety, palpitations, insomnia, poor memory, night sweats.
**Phlegm-Heat** — brain fog, heaviness, excess weight, hot flashes with accompanying dampness.
A skilled TCM practitioner will identify your specific pattern through pulse diagnosis, tongue observation, and clinical interview — and prescribe accordingly.
---

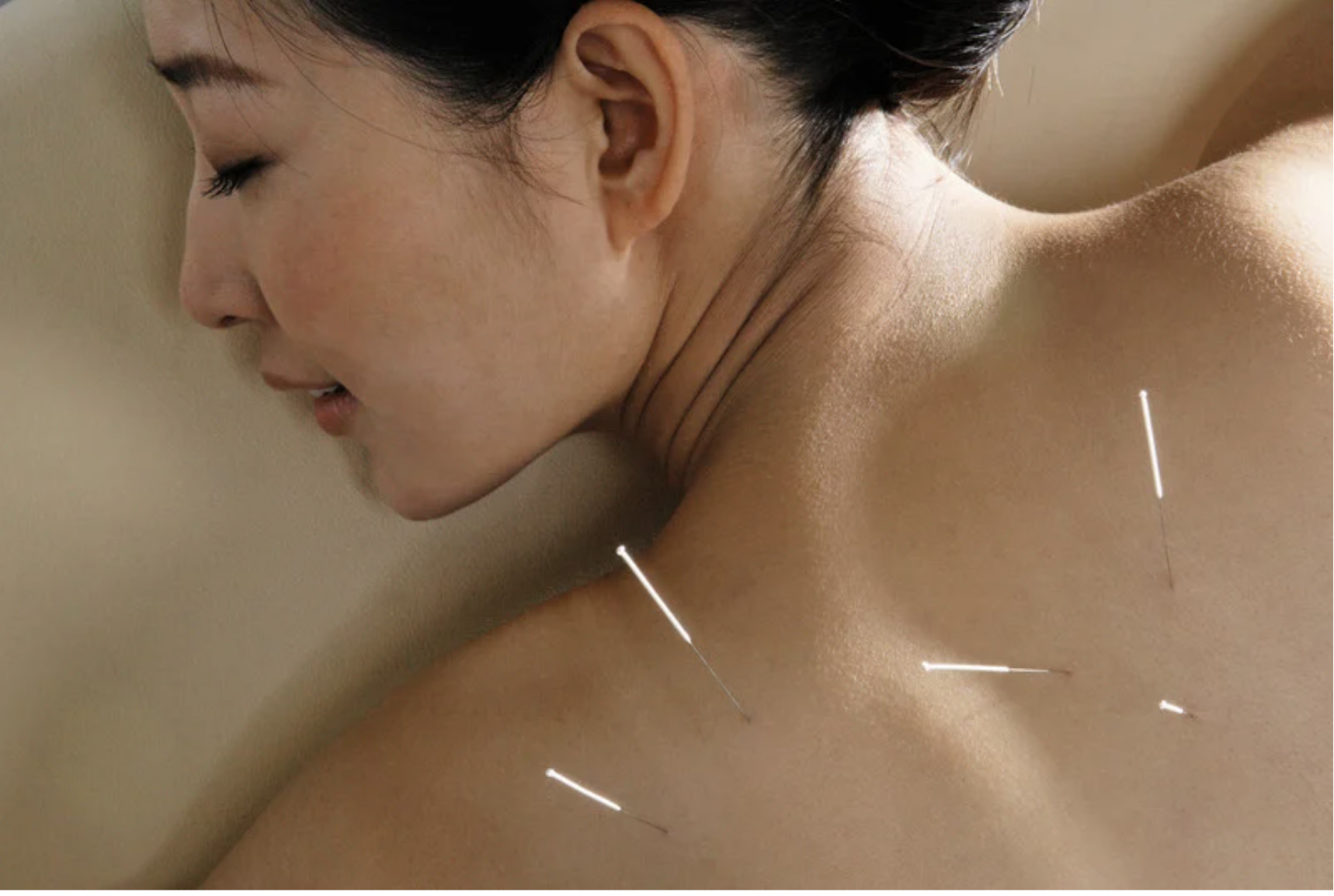
## Acupuncture: The Most Researched TCM Intervention
Acupuncture for perimenopause symptoms has been studied in multiple randomized controlled trials and several systematic reviews. The evidence is stronger than most women realize.
### Hot Flashes and Night Sweats
A landmark 2019 study published in BMJ Open found that a course of 8 acupuncture sessions significantly reduced hot flash frequency, with effects persisting for up to 6 months after treatment ended. The average reduction was 36%, with some participants experiencing far greater relief.
A 2016 Cochrane review analyzed 16 RCTs and confirmed that acupuncture produces meaningful reductions in vasomotor symptom frequency and severity compared to both sham acupuncture and waitlist controls.
### Sleep and Anxiety
Acupuncture has well-documented effects on sleep quality through its influence on melatonin, GABA, and beta-endorphin pathways. For perimenopausal insomnia specifically, a 2020 meta-analysis found statistically significant improvements in sleep onset, maintenance, and total sleep time.
The anxiolytic effects of acupuncture are mediated in part through the HPA axis — the same system disrupted by declining estrogen. This is not a coincidence.
### Joint Pain and Musculoskeletal Symptoms
Acupuncture's analgesic effects are among its most robustly supported mechanisms, involving endorphin release and modulation of inflammatory cytokines. For the joint pain and musculoskeletal stiffness that frequently accompany perimenopause, acupuncture provides relief that does not require pharmaceutical intervention.
### Frequency and Course of Treatment
A typical treatment course for perimenopause is 8–12 sessions, usually twice weekly initially, then weekly as symptoms stabilize. Effects are cumulative — single sessions produce minimal lasting change. This is not acupuncture's limitation; it reflects the biological reality that hormonal recalibration requires sustained therapeutic input.
---

## Chinese Herbal Medicine
Chinese herbal medicine for perimenopause is prescribed as individualized formulas — combinations of 8–15 herbs tailored to your specific pattern. This is categorically different from taking a single supplement.
### The Evidence Base
A 2016 systematic review published in Climacteric analyzed 19 randomized controlled trials of Chinese herbal medicine for menopausal symptoms. It found comparable effectiveness to menopausal hormone therapy for vasomotor symptoms, with a favorable safety profile.
The formulas studied most extensively include:
**Kun Tai capsule** — a proprietary formula showing significant reduction in Kupperman Menopausal Index scores in multiple trials.
**Liu Wei Di Huang Wan** — the foundational formula for Kidney Yin Deficiency. Addresses hot flashes, night sweats, lower back weakness, and urinary symptoms.
**Zhi Bai Di Huang Wan** — Liu Wei Di Huang Wan with added heat-clearing herbs for more pronounced vasomotor symptoms.
**Xiao Yao San / Dan Zhi Xiao Yao San** — the primary formula for Liver Qi Stagnation presentations with emotional volatility, irregular cycles, and breast tenderness.
**Gui Pi Tang** — for Heart-Spleen Deficiency presentations, particularly insomnia, anxiety, palpitations, and fatigue.
These formulas require modification by a practitioner. Taking the base formula without adjustment for your individual presentation is a common mistake that reduces effectiveness.
## Moxibustion
Moxibustion applies heat to acupuncture points using burning moxa (dried mugwort). It is particularly effective for Yang-deficient presentations: fatigue, chilliness, depression, low libido, and weight gain.
Specific points — Shenque (CV8), Guanyuan (CV4), and Zusanli (ST36) — are frequently used for hormonal support and immune regulation. Moxibustion can be learned for home use between clinic sessions, making it a practical tool for ongoing self-care.
## Auricular Acupuncture
Auricular (ear) acupuncture maps the entire body onto points on the outer ear and can be used as a standalone treatment or complement to body acupuncture. For perimenopause, auricular acupuncture is particularly useful for:
- Hot flash reduction between clinic sessions
- Anxiety management
- Sleep support
- Appetite and weight regulation
Semi-permanent ear seeds (small seeds or pellets placed on auricular points with tape) allow women to stimulate points at home between appointments, extending treatment between sessions.
## Tuina (Chinese Medical Massage)
Tuina applies pressure, friction, and manipulation to acupuncture points and meridians. For perimenopausal women, Tuina addresses:
- Muscle tension and joint stiffness
- Liver Qi Stagnation (physical manifestations of emotional holding)
- Circulatory stagnation
It is often integrated into a treatment session alongside acupuncture and can be partially self-administered using acupressure techniques between appointments.
---

## Finding the Right Practitioner
A licensed TCM practitioner is essential. Pattern differentiation — the core diagnostic process — requires clinical training and supervised practice that cannot be replicated from a book or app.
In the United States, licensed acupuncturists (L.Ac.) have completed 3–4 year master's programs and passed national board examinations administered by the National Certification Commission for Acupuncture and Oriental Medicine (NCCAOM). Doctors of Oriental Medicine (DOM or DAOM) have completed additional doctoral-level training.
When selecting a practitioner, ask specifically about their experience with perimenopause and menopausal transition. Not all TCM practitioners focus on women's health — finding one with this specialization will significantly affect outcomes.
TCM does not offer symptom management as a separate goal from overall health optimization. The same treatment that reduces your hot flashes also addresses your sleep, your anxiety, your cognitive function, and your long-term Kidney essence — because in TCM, these are not separate problems.
That integration is its most valuable quality.
---
*This post is for educational and informational purposes only. It is not a substitute for personalized medical or TCM advice. If you are experiencing significant perimenopause symptoms, consult both a menopause-informed clinician and a licensed TCM practitioner.*